Share:
Last month, Clinical Corner distinguished between outcomes and outcome measures and highlighted some of the results of a survey with therapists practicing in seating and mobility in Canada regarding the use of outcomes and outcome measures. See Outcomes and Outcome Measures in Seating and Mobility: Current Practice to refer to that article. This month, Clinical Corner will continue its focus on outcome measures with a look at key considerations when selecting outcome measures.
Relevance
Before we begin to highlight key considerations in outcome measures for seating and mobility, let's review why the use of outcome measures, rather than describing outcomes, is important in seating and mobility. The use of an outcome measure may help with equipment selection as it may provide objective evidence regarding the effectiveness of the technology that is selected for a client. In addition, the use of an outcome measure may help to provide objective evidence to funders when advocating for certain equipment on behalf of clients. The Rehabilitation Engineering & Assistive Technology Society of North America (RESNA) Wheelchair Service Provision Guide (2011) states that "Standardized and validated measures should be used whenever possible to allow comparison of identified variables before, during and after the process. Standardized tools also allow for comparisons across clients, types of equipment, and various service delivery models" (p. 12). The RESNA Wheelchair Service Provision Guide (2011) further states: "Professionals involved in the provision of wheelchairs should apply outcome measures to raise the standard of practice, to support evidence-based practice, and to improve the level of accountability." (p. 12)
Key Considerations
One of the first things to consider when selecting an outcome measure to use in seating and mobility practice is to identify the area that is to be measured (O'Reilly & Patro, n.d.). The International Classification of Functioning, Disability and Health (ICF) can be used to classify the focus of the measurement tool. See below for the ICF Model.
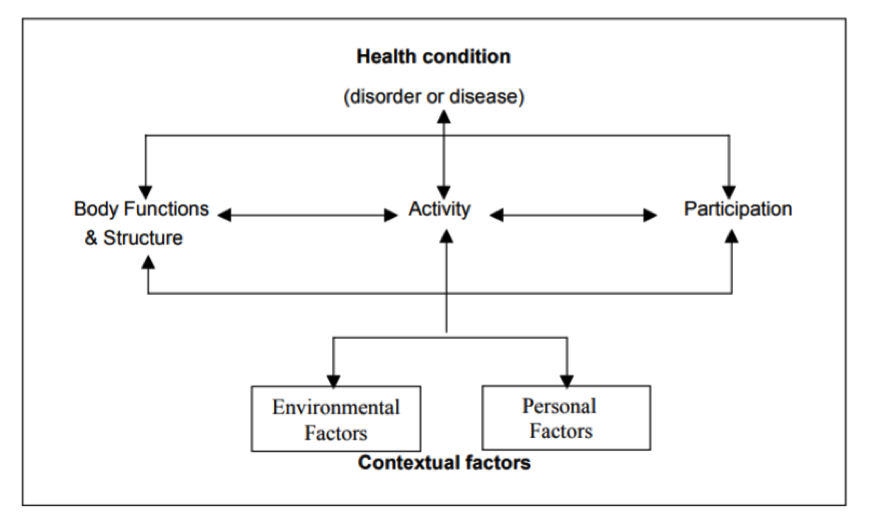
(World Health Organization, 2002, p. 9)
The focus of an outcome measure used in seating and mobility may relate to:
- Body functions: physiological and psychological functions
- Body structures: anatomical parts of the body
- Activity: tasks or actions completed by individuals and any activity limitations experienced. This measures an individual's capacity, or what the individual can do when using the mobility device. Often, this type of evaluation will be measured in a controlled environment.
- Participation: involvement in life situations and any participation restrictions experienced. This measures what an individual typically does in their own environment.
- Environmental factors: positive and negative factors in the environment that act as barriers or facilitators to activity and participation (e.g., architectural characteristics, climate, terrain, social structures, etc.)
- Personal factors: factors, such past and present experiences, that influence how disability is experienced by the individual
(World Health Organization, 2002)
Other considerations in selecting an outcome measure are the degree to which the outcome measure is reliable, valid and responsive to change. (O'Reilly & Patro, n.d.) The cost of the measurement tool may be a factor. Some measures may require a license to utilize while others are free to download from the internet. Implementation of the outcome measure also may be a consideration. Factors such as the amount of time or space required to administer the outcome measure must be considered. In addition, the need for training to administer the outcome measure or the inclusion of clear, standardized instructions must be evaluated. If the outcome measure is a client self-report, the therapist must consider the amount of time required to complete the self-report and whether or not the measure is meant for the client to complete independently. (O'Reilly & Patro, n.d.)
A future Clinical Corner article will describe some common seating and mobility outcome measures.
As always, please provide your comments, questions and suggestions regarding Clinical Corner. Please email me at Sheilagh.Sherman@sunmed.com. I look forward to hearing from you!
Sheilagh Sherman, BA, BHScOT, MHM, OT Reg. (Ont.)
Clinical Educator
Sunrise Medical Canada
References:
- O'Reilly N. & Patro, A. (n.d.) Wheelchair Related Outcome Measures. Retrieved from https://www.physio-pedia.com/Wheelchair_Related_Outcome_Measures
- RESNA. (2011). RESNA Wheelchair Service Provision Guide. Retrieved from http://www.resna.org/
- World Health Organization. (2002). Towards a Common Language for Functioning, Disability and Health. ICF. Retrieved from https://www.who.int/
Note: The content of this article is not meant to be prescriptive; rather, it is meant as a general resource for clinicians to then use clinical reasoning skills to determine optimal seating and mobility solutions for individual clients. Sheilagh is unable to answer questions from members of the general public. Members of the general public are directed to their own therapists or other health care professionals to ask questions regarding seating and mobility needs.
This article is © Sunrise Medical, Inc., 2019 and cannot be copied, distributed, or otherwise reproduced in whole or in part without the express written permission of Sunrise Medical Canada.